Article Summary
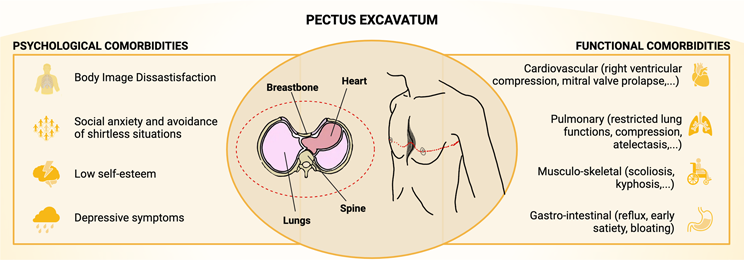
Pectus excavatum and Poland syndrome, although embryologically distinct conditions, share a visible alteration of chest wall morphology, which is the main reason patients seek treatment. The article highlights that cardiopulmonary impairment is often limited or absent, whereas the aesthetic and psychosocial impact is usually predominant.
Historically, treatment relied on thoracic remodeling techniques such as the Nuss and Ravitch procedures, which aim to correct the skeletal structure. However, these approaches are invasive, medically and economically costly, and associated with non-negligible morbidity.
Recent advances in 3D imaging, computer-aided design (CAD), and the manufacturing of patient-specific implants have enabled the development of alternative approaches based on morphological reconstruction with custom-made implants. These techniques provide precise, individualized correction with a less invasive profile.
The article emphasizes one central point: no single technique can be considered superior in all cases.
Treatment choice must be individualized, depending on:
- anatomical characteristics
- the presence of any functional impairment
- patient expectations
Accordingly:
- thoracic remodeling techniques remain indicated in cases of severe deformity with functional impact
- custom-made implants represent a relevant alternative when the main indication is morphological correction
Finally, the authors underline the lack of robust comparative studies and the need for higher-quality evidence to better guide clinical decision-making.
Understanding of the Approaches
Nuss
Goal: Push the sternum outward
Approach: Internal metal bar
Key point: Acts on bone structure
Ravitch
Goal: Reshape cartilage and sternum
Approach: Open surgery
Key point: Structural correction
3D Custom-Made Implants
Goal: Fill the chest depression
Approach: External implant
Key point: Morphological correction
About Prof. Thiessen’s Department
Prof. Filip Thiessen is a board-certified plastic surgeon and Professor at the University of Antwerp. He practices notably at Antwerp University Hospital (UZA) as well as in several specialized centers in Belgium.
His department is recognized for its expertise in advanced reconstructive surgery, including chest wall reconstruction, breast reconstruction, and personalized techniques. Trained in Europe and internationally (England, France, and Chile), Prof. Thiessen combines an academic approach, technological innovation, and patient-centered care.
Actively involved in clinical research and teaching, he develops approaches based on precision and customized planning, particularly through the use of 3D technologies. His team is committed to surgical excellence and innovation in personalized reconstruction.