When considering pectus excavatum surgery, the first question is not “what techniques exist?”, but rather: what is my problem, and which surgery is suited to my situation?
Between the semi-closed Nuss technique, the open Ravitch method and 3D custom-made implants, the choice depends on several medical and personal criteria.
Is it always necessary to have surgery for pectus?
Pectus excavatum, in all its forms, is common: it affects around 1 in 500 births. In the majority of cases, it is only slightly symptomatic or not symptomatic at all, and not all patients necessarily wish to undergo surgery.
The indication for surgery is therefore mainly based on two major criteria:
- a functional impact, with cardiac or respiratory insufficiency confirmed at rest or during exercise;
- a significant aesthetic and psychological impact, with disturbance of self-image and social relationships.
If there is any doubt about the functional impact of pectus, the first step is a precise clinical assessment in order to determine whether the cardiac or respiratory disorders justify a more invasive structural correction.
Cardiac evaluation
Transthoracic echocardiography is the first-line dynamic examination used to assess the cardiac impact of pectus excavatum.
Its purpose is to look for:
- compression of the left ventricle;
- evaluation of systolic and diastolic function;
- analysis of cardiac filling;
- investigation of any associated valvular abnormality, such as mitral valve prolapse.
It is a dynamic, non-invasive, accessible and reproducible examination. It is the basic cardiac examination used to document possible cardiac impact, at rest or during exercise.
Cardiac MRI, for its part, makes it possible to analyse the anatomical and functional impact of funnel chest on the heart, but it remains a static examination, like a CT scan.
Respiratory evaluation
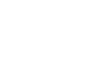
CPET (Cardiopulmonary Exercise Testing) is the most sensitive and most discriminating examination for assessing the functional impact of pectus excavatum.
However, its usefulness is debated by some authors. Gonzalez et al.(1) thus conclude in Pediatric Surgery International that patients who underwent pulmonary function tests did not differ significantly from those who did not undergo them for most of the structural and functional measures of the deformity and cardiopulmonary function.
Furthermore, people who do little or no physical activity may be more short of breath, not directly because of the pectus, but because of deconditioning linked to the limitation of their activity. This is then referred to as a peripheral deficit linked to a pathology.
In which cases should bone or orthopedic surgery be considered?
The Nuss technique: for which situations?
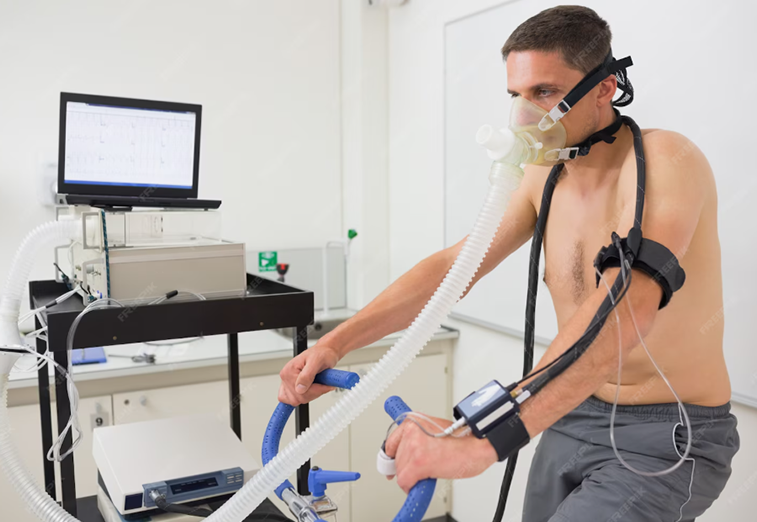
The Nuss technique(2) is a thoracic surgery consisting of placing one or more curved metal bars between the heart and the sternum in order to push back the chest wall and correct the shape of the bony thorax. It is relevant in young adults when the sternal deformity is centered, symmetrical and causes a real functional impact.
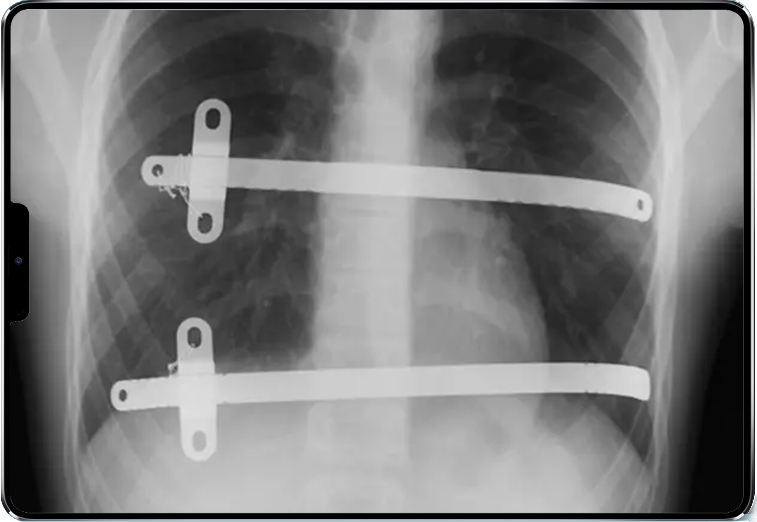
Characteristics of the semi-closed endoscopic technique:
- small lateral skin incisions, around 5 cm on each side of the thorax;
- insertion of one or more preformed curved metal bars under optical guidance behind the sternum, near the heart;
- sometimes the placement of several parallel or crossed bars;
- 90° rotation to exert anterior pressure on the sternum and ribs;
- possible fixation to the ribs by sutures or stabilizers;
- removal of the bar 2 to 3 years after implantation.
The operation generally lasts 1 to 2 hours, and hospitalization lasts between 4 and 7 days.
The Nuss technique is based on the ability of the thorax to be remodelled by progressive mechanical stress. It is therefore more favourable in young patients whose chest wall is still flexible. With age, sterno-costal rigidity increases, making correction more demanding and associated with more painful postoperative recovery as well as a higher rate of complications. Several studies have shown that outcomes in adults are less favourable than in adolescents, particularly in terms of postoperative pain and complications (Pilegaard HK, Annals of Cardiothoracic Surgery, 2016(3)).
Advantages and disadvantages of Nuss
The Nuss technique does not involve cartilage resection, allows progressive straightening of the thorax and generally leaves less visible lateral scars.
Nevertheless, it involves postoperative pain, two surgical interventions and a delicate intrathoracic procedure. The creators of the technique themselves acknowledge the possibility of major risks when it is not perfectly mastered, even if these complications become rare with the surgeon’s experience.
These risks are also mentioned by advocates of open techniques. De Wolf et al.(4) thus remind us that cardiovascular morbidity and mortality linked to minimally invasive repair using a Nuss bar seem more severe than those observed during open surgery.
MIRPE (Minimally Invasive Repair of Pectus Excavatum(5)) does in fact involve passing a metal bar behind the sternum, in an anatomical space very close to the heart and lungs, which represents a potentially serious, even life-threatening, risk, although rare.
In addition, the functional benefit is not systematically demonstrated. Castellani et al.(6) already indicated in 2010 that, according to their data, pectus repair was not followed by an improvement in pulmonary function or exercise performance. Del Frari et al.(7) in 2022, then Dupuis et al.(8) in 2024, point in the same direction by finding no significant improvement in cardiopulmonary parameters and exercise capacity after bar placement and removal.
The Ravitch technique: in which cases?
The Ravitch technique(9) is an open thoracic surgery for immediate structural remodelling. It is indicated for complex chest wall deformities, asymmetrical deformities, associated with other costal abnormalities, with functional impact, particularly in adults.
Although the Ravitch technique can be performed at any age, it is often indicated in older patients or in patients with complex deformities, because thoracic rigidity limits the effectiveness of minimally invasive techniques. However, in adults, this surgery remains invasive and is associated with non-negligible morbidity, linked in particular to cartilage resection and bony stabilization. The choice of this technique therefore depends heavily on age, thoracic rigidity and the complexity of the deformity (Fonkalsrud EW, Annals of Surgery, 2000(10)).
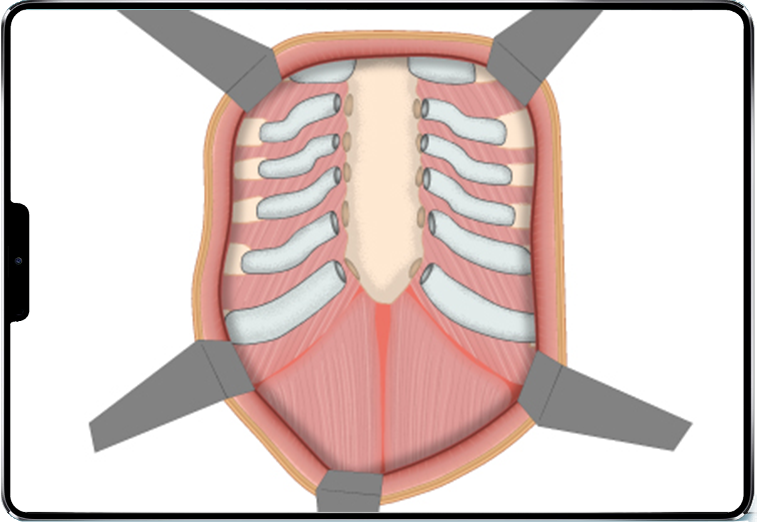
Its characteristics are as follows:
- a wide anterior incision, often submammary or median;
- detachment of the pectoral muscles;
- resection of the deformed costal cartilages and sectioning of the sternum;
- repositioning of the sternum in its anatomical position;
- stabilization with bars and osteosynthesis screws;
- removal of the bar 2 to 3 years after implantation.
The operation generally lasts 2 to 3 hours and hospitalization lasts between 5 and 7 days.
Advantages and disadvantages of Ravitch
The Ravitch technique allows direct remodelling of the thorax and reduces the risk of cardiac injury compared with the retrosternal passage of the Nuss bar. It can be particularly useful when the pectus presents cardiac or pulmonary impact and is associated with other thoracic pathologies, such as cartilage torsion, cartilaginous hypertrophy or costal hypoplasia.
However, it is a heavier (2 operative stages) and invasive surgery, with significant muscular alteration and therefore a recovery time and postoperative pain.
Furthermore, the thoracic stabilization system after correction may also prove to be defective. Berthet et al.(11) thus describe complications of bar rupture, displacement or fracture. Sharma et al.(12) explain that repeated mechanical stresses related to breathing, such as traction, compression or torsion, can cause material fatigue and lead to fracture.
The authors also report a release of titanium particles into the body, which may lead to metallosis. These failures may represent a danger to vital organs and justify close monitoring of the operated patient.
3D custom-made implants: the alternative
When funnel chest is mainly an aesthetic concern, a less invasive solution may be considered: filling with a 3D custom-made silicone rubber implant, designed from a 3D scan. This solution is intended for deformities without major functional context but responsible for significant psychological and social discomfort.
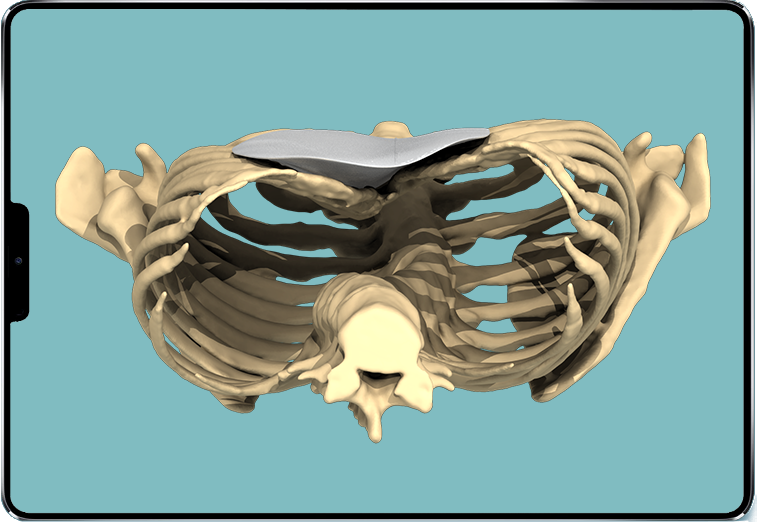
- no structural modification of the chest wall;
- a solution suited to patients aged 15 to 70;
- suitable for symmetrical as well as asymmetrical forms;
- generally simpler and less painful postoperative recovery;
- a single intervention;
- immediate and complete filling of the hollow;
- a permanent non-degradable implant;
- a possible solution in revision after failure of other techniques.
The operation generally lasts 1 hour, with discharge either the same day or the following day. Return to work takes place 15 days after the operation and return to sport 3 months later (1 year for sports involving the pectorals more heavily).
Advantages and disadvantages of the 3D implant
The 3D implant is therefore a less invasive surgical technique, without opening the thorax and therefore far from the heart. Only one intervention is necessary and provides an immediate result after a short operating time and simple postoperative recovery relieved by simple painkillers.
It is also the technique to be preferred for correcting imperfect pectus correction results, known as revision cases. Chavoin et al.(13) explain that because the technique is based on filling the defect rather than remodelling the chest wall, it can be offered both to adults and to adolescents at the end of growth, without any specific increase in age-related risk. It therefore constitutes a particularly relevant alternative in adult patients, in whom bony techniques are more demanding or less well tolerated.
This approach aims to correct the visible hollow by precise and immediate filling, without major thoracic surgery. It is suited to many types of deformities(14): mild pectus, pectus arcuatum, asymmetrical forms, deep deformities, in both men and women, from the end of puberty onwards. There is no strict age limit if the patient is in good general health.
It should nevertheless be specified that in the event of possible functional cardiac or respiratory impact, the implant technique does not correct the bony structure of the thorax. It is indicated mainly in aesthetic forms and requires rigorous prior analysis to establish the correct indication.
How to choose the right surgery?
The choice of operation depends above all on whether or not there are objectively confirmed functional symptoms.
As Bastien L., former patient of Prof. Chavoin, former head of the plastic surgery department at Toulouse University Hospital, testifies, there is not a single “best” operation. Above all, there is a right indication for the right patient.
“I tried building up my pectoral muscles, but it did not lead to any improvement.
I therefore researched the different surgical techniques, such as sternochondroplasty, but most of them seemed too heavy to me, with too many risks and too much hospitalization and recovery time for an aesthetic objective.
Dr. Chavoin’s implant surgery was for me the best and most reasonable solution.”
Conclusion
If the deformity causes real cardiac or respiratory discomfort, thoracic surgery such as the Nuss or Ravitch technique may be indicated. This discomfort must be confirmed by appropriate examinations carried out in an independent cardiology or respiratory functional assessment centre. Given the complexity of these procedures, the choice of a highly experienced surgeon is essential.
If the objective is mainly aesthetic, correction with a 3D custom-made implant constitutes an effective and less invasive alternative.
A specialist consultation makes it possible to assess precisely the most suitable solution. Do not hesitate to consult a referral surgeon, plastic, thoracic or paediatric, after the advice of your general practitioner.